|
When the rectum is prolapsed, it has gone past the anal sphincter, and this allows stool and mucus to pass in an uncontrolled fashion. The anal sphincter is a structure made of a number of muscles that allow one to hold on to their stool when they have the urge to move their bowels. Once a prolapse is apparent, fecal incontinence (inability to control gas, liquid or solid BM) occurs in 50-75% of cases and is likely due to a number of factors. Rectal prolapse may be confused with significant hemorrhoid disease and can even be confusing at times to physicians not frequently evaluating and treating this problem. Until the prolapsed rectum goes back in, patients may feel like they are “sitting on a ball”. Patients may later describe a mass or “something falling out” that they may have to push back in following a BM. 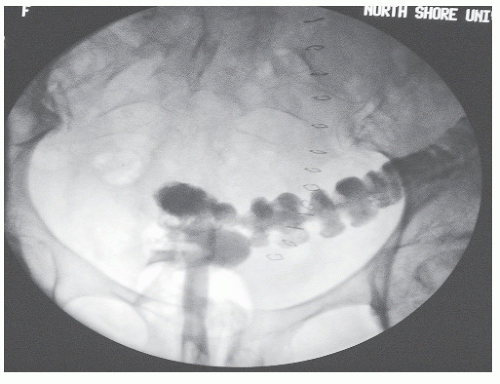
Initially, the prolapse comes down with a bowel movement (BM) and then returns to its normal position. 
Rectal prolapse tends to present gradually. Some have assumed that the development of rectal prolapse is a consequence of multiple vaginal deliveries however, up to 35% of patients with rectal prolapse have never had children. Chronic constipation (infrequent stools or severe straining) is present in 30-67% of patients, while an additional 15% experience diarrhea. While a number of factors have been shown to be associated with rectal prolapse development, there is no clear cut “cause” of rectal prolapse. In these younger patients, there is higher rate of autism, developmental delay, and psychiatric problems requiring multiple medications.Īlthough an operation is not always needed, the definitive treatment of rectal prolapse requires surgery. Most women with rectal prolapse are in their 60’s, while the few men who develop prolapse are much younger, averaging 40 years of age or less. This condition affects mostly adults, and women over 50 years of age are six times as likely as men to develop rectal prolapse. Overall, rectal prolapse affects relatively few people (2.5 cases/100,000 people). However, it can be quite embarrassing and often has a significant negative impact on patients’ quality of life. While this may be uncomfortable, it rarely results in an emergent medical problem. Rectal prolapse is a condition in which the rectum (the last part of the large intestine before it exits the anus) loses its normal attachments inside the body, allowing it to telescope out through the anus, thereby turning it “inside out”. It will address why surgery may have been recommended, what the various treatment options are, what it involves and how it may help patients. Treatment of this condition may often require surgery, and this patient education material is intended for patients with rectal prolapse who are considering or have been recommended surgery. This information may also be useful to the friends, families, and caregivers of patients dealing with rectal prolapse. This patient education piece is designed to help improve patients’ understanding regarding rectal prolapse, specifically its presentation, evaluation and treatment. Rectovaginal fistula stapled closure transperineal repair.Print this brochure Rectal Prolapse Expanded Version 
The initial results are encouraging, suggesting the need for a more formal prospective assessment of this technique as part of a randomized trial for the management of low- and mid-vaginal fistulas. Stapled transperineal repair of RVF appears safe and effective. The mean postoperative Wexner score was significantly improved when compared with the preoperative scores (mean preoperative vs postoperative Wexner scores 3 vs 1, respectively P =. Over a median follow-up of 6 months (range 3-33 months), no case was encountered with recurrence. 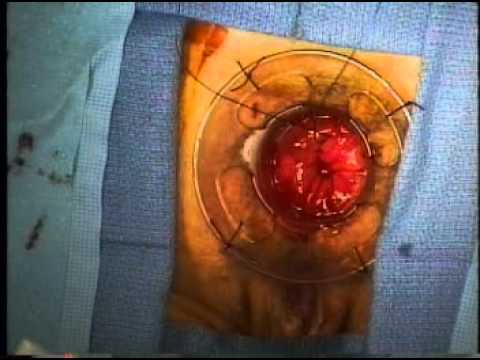
Concomitant levatorplasty was performed with 4 patients and sphincteroplasty with 2 patients. The estimated blood loss during operation was 24 ± 14 mL. The mean operative time was 119 ± 42 minutes. Seven consecutive RVF patients underwent stapled transperineal repair. This study is designed to assess the safety, efficacy, and postoperative outcomes of stapled transperineal repair in management of rectovaginal fistula (RVF).Ī prospective database of patients with RVF undergoing stapled transperineal repair between May 2015 and December 2017 was established and studied retrospectively.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
